Debunking The Myth: Low Carb Diet Reduces Thyroid Function
-
Carnivore “guru” claims absence of carbohydrates ruined his thyroid.
-
Guru refuses to provide medical records substantiating his story.
-
Physiologist explains why low-carb/no-carb diets reduce the T3 hormone without any adverse metabolic consequences.
-
Why people in ketosis, consuming no vitamin C, don’t get scurvy.
By Dave Champion, Ph.D. | July 10, 2021
I recently came across the claim – presented most adamantly – that living in ketosis, the very definition of which is very low carbohydrate intake, results in impairment of proper thyroid function. The specific assertion was that 2 years of “Keto” had “wrecked” his thyroid.
There are all sorts of bizarre non-factual claims made on the internet concerning…well…just about anything. I usually just shake my head and move on. However, in this case, due to who was making this claim I feel compelled to set the record straight.
The assertion was put forth by a social media influencer with a significant following. He claims to be a supporter of the Carnivore style of eating, while illogically claiming one must also eat carbs to prevent improper thyroid function. The influencer making the claim goes by the internet handle, “Carnivore Aurelius” (hereafter, CA).
CA is not a person. CA is a company in Wyoming employing 23 workers and selling packaged meat “crisps”. I share CA’s identity not to begin an “influencer war”. That’s the last thing upon which I have time to waste. Rather I share the identity to ensure people who care about their health steer clear of marketing gurus (which CA most certainly is) putting out falsehoods for no loftier purpose than distinguishing themselves in an over-saturated social media marketing environment.
CA pretends to be a person and attempts to justify hiding behind a pseudonym with statements such as, “Pseudonymity is the ultimate enabler of free speech.” That is of course an absurd and self-serving assertion. I engage in free speech each and every day across numerous social media platforms using my own name. Though I promote the “Dr Reality” brand, it is always combined with my true name, appearing as “Dr Reality – Dave Champion”. I have done this from day-1, and will always do so, because I believe a significant element of what makes free speech so powerful is personal accountability. Credibility suffers greatly when no one is accountable for what is being said.
Before I jump into the physiology of CA’s claim, allow me to share how my background conversation went with CA.
The characterization made by CA was that over a 2-year period Keto had “wrecked” his thyroid. (Keep in mind CA is a business, not a person.) Since “wrecked” is not a medical diagnosis I reached out to CA to see if there was some confusion. Perhaps the employee tasked with making the company’s Instagram posts (which is where the claim was first seen) had a thyroid issue and mistakenly believed it was associated with ketosis.
I started by inquiring how CA could make such a claim in light of the fact that millions of people living in ketosis have no such issue, and CA was the only ‘person’ (who should, in theory, know better) making that claim. I was surprised at the response I received, which involved making more unsupported claims, and offering a single study about T3 (one the two primary thyroid hormones) reduction in people with medically induced hyperglucagonemia. If you’re thinking, “How does that have anything to do with ketosis?”, you’re using your noodle. Hyperglucagonemia has nothing to do with ketosis.
When I pointed out there is no association between hyperglucagonemia and ketosis, CA went on to double down with more unsupported statement such as, “Lots of people on Keto have low T3”, they [people on Keto] have “high cortisol”, they are “losing their hair”, and they have a lot of “subclinical signs”. Subclinical signs? Of what, exactly?
At this point I was frustrated with CA’s unprofessionalism. I felt like I was speaking with a child who just wanted to be “right” rather than factual. Time is always in short supply for me so I cut to the chase. I asked him (whoever it was at the company with whom I was communicating) to email me the results of the following thyroid function tests (TFT) he’d had; TSH, T4, T3, free T3, reverse T3, antibody (looking for things like Hashimoto’s disease), and RIU. It is at that point all conversation ended. Phrase another way, when I requested EVIDENCE of the alleged Keto-related thyroid issue CA fell silent. I understand. It’s tough to provide evidence that doesn’t exist.
I imagine you already doubt CA is a credible source of information. But let’s go a step further and explore the actual physiology. (Just as in “Body Science”, I’ll keep it easy to understand.)
The thyroid is an integral part of your body’s endocrine system. The endocrine system is inarguably one of the most complex systems in the human body. It is a balancing act involving numerous interrelated feedback loops, with a confounding number of variables, a seemingly endless string of chemical and bioelectrical sequences that would take years of focussed study for one person to fully comprehend. All of which affects every tissue in your body.
Before I get into thyroid-specific info, let me remind you that the “normal range” for every bodily substance is the result of research performed on bodies operated exclusively in the toxic state of glucosis. (99.9% of the world’s population.) Despite mankind living in ketosis from birth to death for millions of years (until the First Agricultural Revolution), modern medical science had never investigated or determined what is the “normal” range concerning…anything…for a body in ketosis. (I explain mankind’s inadvertent and health-diminishing journey from ketosis to glucosis in “Body Science”.)
As an example, Dave Feldman’s work at cholesterolcode.com has shown that within a subset of people in ketosis there is a type identified as “Lean Mass Hyper-responder” (LMHR) who have (among other factors) a LDL level so high it would make a cardiologist go apoplectic. But for the LMHR that high LDL level is neither harmful nor abnormal. It is completely normal. (I explain the truth about cholesterol in “Body Science”.)
Another example is fasting blood glucose level. For a person in the toxic state of glucosis, “normal” is 99 mg/dL or below. In other words, 99 is the top of normal. If you exceed that, it’s no longer considered “normal.” In fact, the medical industry interprets any number above 99 as a sign you are pre-diabetic. But is that true of a person living in ketosis? No! Due to a natural and healthy ketosis phenomenon called “glucose rejection”, it is normal for a ketosian’s fasting blood glucose level to be several points above the highest “normal” for people in glucosis. In other words, 103, 104, or 105 is abnormal for people in glucosis, but perfectly normal for a person who has been in ketosis for some time.
Yet another example is the issue of vitamin C and scurvy. A body in the toxic state of glucosis must have a minimum intake of vitamin C (a floor of 10 mg, with 50 mg recommended) or it will experience the onset of scurvy. A body in ketosis can exist with only trace amounts of vitamin C found in meat, and never get scurvy. An ordinary 8-ounce store-bought steak in the U.S. has less than 3.6 mg of vitamin C; well beneath the minimum needed to prevent scurvy. Yet people in ketosis who eating just meat never get scurvy.
The point we want to keep in mind as we move forward is what has been determined to be “normal” for a body in glucosis may have little bearing on what is normal for a body in ketosis. You’re going to see a thyroid-specific example of that momentarily.
Earlier I stated that the thyroid endocrine system has “a confounding number of variables.” Those variables do three things.
1. Makes it difficult for a general practitioner to be certain whether a patient has a thyroid problem. In the U.S. general practitioners traditionally order the TSH test and a T4 test, making the diagnosis from just those 2 tests. In reality, those two tests, taken together, are merely an indictor and do not provide enough data to establish whether the patient actually has a thyroid-related endocrine problem.
2. Means a fully fact-based determination concerning a thyroid-related endocrine problem needs to be made by a specialist in the field; an endocrinologist.
3. Makes it essentially impossible for an ordinary person to self-diagnose a thyroid problem.
This may give you a better idea why the conversation with CA went dark as soon as I asked for test results. None exist. CA’s claim was either a marketing stunt to distinguish itself from its competitors by making a controversial (and false) claim, or someone at CA was simply doing what cannot be done; self-diagnosing a perceived thyroid issue.
Are there things a person can do that adversely affect thyroid function without regard to glucosis or ketosis? You bet. A key element powering thyroid function is iodine. In the U.S., most people get their iodine from table salt, which almost universally has had iodine salts added since the 1980s. A person who chooses to drastically reduce salt intake, and also does not eat foods with much iodine, will experience thyroid issues because a foundational element needed by the thyroid is not present in the body. (Foods naturally high in iodine are seaweed, cod, dairy products, oysters, and eggs.)
If a person has the gene mutation associated with Hashimoto’s disease, but the disease has not yet manifested, a change in dietary pattern that involves a sudden spike in iodine intake can cause the onset of Hashimoto’s.
Then there is the impact other endocrine hormones can have on the primary thyroid hormones. An example of this is elevated estrogen. Elevated estrogen can increase the body’s production of Thyroid-Binding Globulin (TBG) which will in turn decrease the amount of active T3/T4 in the blood. (Bound T3/T4 is inactive.)
In terms of living in ketosis, pay attention to this next matter.
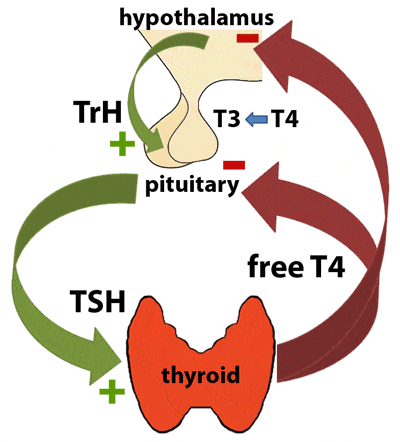
An increase in free fatty acids in the blood will displace TBG, which decreases binding, thus allowing for an increase in the level of “free” (active) T3/T4. BUT…that increase will be short-lived and levels will quickly return to the proper balance. Why? Remember earlier I said the endocrine system is a balancing act involving numerous interrelated feedback loops? This is a prime example. Increased levels of T3/T4 will signal the pituitary gland to excrete less Thyroid Stimulating Hormone (TSH), which signals the thyroid to reduce the production of T3/T4, thus restoring the proper balance of free/active T3/T4 and bound/inactive T3/T4 in the blood.
The above sequence will almost certainly occur when a person’s body flips from glucosis into ketosis because the hundred trillion cells of the body then want fatty acids as their energy source (rather than glucose), coupled with the fact that people eating to sustain ketosis are consuming what is seen by the glucosis-centric establishment as very large amounts of dietary fat. (In “Body Science” I provide a fascinating expose´ on the journey and process dietary fat undergoes from your mouth to providing energy to each of your hundred trillion cells!)
What of the generalized claim that people in ketosis have “low” T3? Well…some do. This is exactly the time to recall that “normal” for people in glucosis may not be normal at all for those living in ketosis.
The body is amazing. It knows what it needs and adjusts levels to what it needs. (This is accomplished through an incalculable number of feedback loops and internal signaling.) As an example, roughly 2/3 of cholesterol is made within your body, without regard to diet. More significantly, if you eat foods high in cholesterol your body will reduce its own production. If you eat foods low in cholesterol your body will increase its cholesterol production. (In “Body Science” I explain what humans do to themselves that pushes that amazing, elegant, self-regulating system off the rails, leading to chronic disease and premature death.)
If I were to illustrate the dearth of research into how the body operates in ketosis by saying 99.999999% of medical research has been on people in glucosis, with only 0.000001% being done on people living in ketosis, that would be a fairly accurate picture. (The near total blackout on research funding for ketosis is 100% intentional. I explain why in “Body Science”.)
That said, there have been studies with the primary focus on something other than ketosis, yet looking at ketosis tangentially. An example is that the U.S. government doesn’t spend a penny on any meaningful ketosis research except in situations such as Navy SEALS experimenting with ketosis to reduce the occurrence of seizures experienced from extended use of rebreathing devices. (The unavoidable takeaway from the government’s funding decisions is it’s happy to provide any amount of money for ketosis research to improve U.S. war-fighting capabilities, but not a penny to improve the health of the American people.)
One area in which ketosis has been looked at tangentially is epilepsy; specifically as treatment of epilepsy in children. It is here we find some interesting data concerning ketosis and T3 levels. In a 2017 study researchers found children in ketosis experienced an initial increase in TSH in the first 30 days, with TSH returning to its pre-ketosis level over a 12-month period. (When TSH output returned to pre-ketosis level varied from test subject to test subject, ranging from the 2nd to 12th month.)
Interestingly, while TSH initially increased, and then returned to pre-ketosis level, free T3 levels dropped significantly overall. In other words, while TSH output returned to pre-ketosis level, T3 did not. Even more interesting is researchers found no adverse affects resulting from ‘in ketosis T3’ being lower than ‘in glucosis T3’. In other words, while I wouldn’t consider this particular study conclusive, it is certainly indicative that T3 being lower in ketosis than in glucosis is completely natural and is simply the body doing what it does; seeking the balance that maintains proper health.
Is there a physiological explanation as to why T3 levels drop in ketosis. You bet!
T3 plays a key role in glucose metabolism. In other words, if your body is burning glucose for energy the body must make sufficient T3 to facilitate that process. Phrased another way, when your body is fueling its trillion cells by incinerating a toxic over-abundance of glucose in the blood [the very definition of glucosis] then a high T3 level is necessary. When that process stops, and the body is running in the manner for which it is genetically coded – i.e. ketosis – less T3 is needed, thus less T3 is produced.
A simple “observational study” anyone can perform is to witness that the bodies of people who live in ketosis drop all excess body fat. This is the exact opposite of what would be expected if lower T3 levels in ketosians produced hypothyroidism, as is falsely claimed by some.
I know this article has been complex at times despite my best effort to keep the information streamline and easily understandable. In conclusion I’d like to bullet-point what I hope you’ll take away.
- Social media influencers are usually selling something, and that guides their actions. Revenue is their goal and measure of success, not truthfulness. Even if they claim to be all about “good health” it is unwise to put much stock in what they’re saying.
- Mankind lived in ketosis from birth to death for millions of years, until the Agricultural Revolution. (Did they all have thyroid problems? <wink>)
- The toxic state of glucosis is as different from living in ketosis as night is from day.
- The establishment has done no meaningful research on living in ketosis. As such, what is normal and healthy for a body in ketosis has not been determined by rigorous science.
- The minimal amount of establishment research that has been done on ketosis (virtually all being tangential), independent research such as that performed by Feldman [cholesterol.com], as well as common sense observations, informs us we fall into error if we apply glucosis “norms” to bodies in ketosis.
- Thyroid function is far more complex than the average person understands.
- Most MD general practitioners are ill-equipped to settle whether a patient actually has a thyroid problem.
- Attempting to self-diagnosing a thyroid issue is a fool’s errand.
- Dietary issues unrelated to glucosis or ketosis can affect thyroid function, such as an insufficiency of iodine. (A person without this kind of knowledge may attribute a thyroid function problem to a wholly unrelated issue, such as ketosis.)
- Millions of people live in ketosis with zero evidence of thyroid problems.
- No studies exist suggesting a very low-carb or no-carb diet has any adverse effect on thyroid function.
- T3 levels in ketosis are expected to be lower than in glucosis because T3 is no longer needed to facilitate the toxic glucosis cycle.
- Ketosians with measured T3 levels less than the “glucosis norm” do not experience any physiological affects associated with thyroid problems.
- The body knows what it’s doing. Exponentially more so in ketosis, when set free from the toxicity of glucosis. Let it do what it does so elegantly!
I hope you have found this article informative and helpful. If so, you’ll likely find “Body Science” a fascinating life-changing read. https://drreality.news/product/body-science/
Dave’s “Dr Reality” books can be found at https://drreality.news
Subscribe to podcast at https://drreality.news/subscribe-to-podcast/
Dr Reality YouTube channel: https://www.youtube.com/user/davechampiontv

Food for thought, Dave. This isn’t to debate but rather to inform.”
“Other ‘diseases’ have also been associated with specific nutrient deficiencies;
scurvy, for example, is claimed to be caused by a severe vitamin C deficiency.
However, the ‘new’ explanation of disease demonstrates that scurvy can be more
accurately described as a condition that results from oxidative stress and free radical
damage due to a severe antioxidant deficiency.”
Best,
James